Empowering, Life-Changing Therapies for Urinary Incontinence
The loss of bladder control, called urinary incontinence, is common and troublesome for many women. Urinary incontinence can range from small leaks during activities like laughing, coughing or sneezing, to failure to make it to the toilet in time.
What Causes Urinary Incontinence?
Urinary incontinence can be caused by various factors, many of which are out of our control. These include:
- Pregnancy and childbirth
- Genetics
- Menopause
- Pelvic surgery
- Muscles problems in the bladder and urethra
- Weakened pelvic floor muscles or a weak sphincter muscle at the bladder’s neck
- Obesity
- Chronic medical conditions such as diabetes mellitus
- Anxiety and clinical depression
- Urinary tract infections
After pregnancy and childbirth, women who develop stress urinary incontinence due to weakened pelvic floor muscles and hormonal changes may benefit from Kegel exercises that help them strengthen their pelvic floor muscles.
It is important to work with a specialized and skilled professional who can accurately diagnose and treat your urinary incontinence by identifying the underlying cause. This will ensure you receive the most accurate diagnosis and effective treatment plan.
How Do You Treat Urinary Incontinence?
Approximately 80% of people with urinary incontinence can eliminate or significantly improve their symptoms with the appropriate treatment.
- Practice regular Kegal exercises
- Cut down on fluid intake, especially within 3 hours before you go to bed.
- Avoid activities that put pressure on your bladder such as jumping or jogging and take up low impact activities.
- Lose the excess weight because obesity puts pressure on the bladder, and damages urethral structures as well as the pelvic floor.
- Quit smoking and vaping because it can cause a chronic cough which damages the pelvic floor.
- Avoid alcoholic and caffeinated beverages including coffee, energy drinks, teas, and sodas.
What Are the Best Non-Surgical Treatments for Female Urinary Incontinence?
Women’s Wellness Institute of Dallas offers our patients a wide array of treatment options for urinary incontinence involving all available laser platforms (CO2 Laser, radiofrequency, DiVa, Emsella, Emsculpt 360) as well as platelet-rich plasma injections known to improve urinary incontinence symptoms.
Empower RF by InMode
If lifestyle changes and regular kegal exercises fail to improve urinary incontinence symptoms, there is now a cutting-edge technology available to help called Empower RF. By harnessing the safe, effective power of radiofrequency waves, the Empower RF technologies gently target sensitive tissue with waves of restorative thermal energy. The Empower platform by Inmode utilizes three different handpieces to provide an FDA cleared option for women with urinary incontinence, especially those who wish to avoid a bladder mesh surgery.

Votiva®
The Votiva handpiece delivers comfortable bipolar radiofrequency waves to the vaginal canal to increase collagen production and improve blood supply. The first of three steps to achieve optimal non-invasive urinary incontinence treatment, this comfortable 30 minute procedure involves no downtime or significant restrictions. A Votiva therapy program is customized to each patient based on severity of symptoms, medical history, and physical exam.
Benefits of Votiva:
- RF stimulates collagen production, which naturally rejuvenates vaginal tissue and can improve internal structural stability
- Reduces mild to moderate stress urinary incontinence and urge incontinence/overactive bladder that can naturally occur due to childbirth, aging, and genetics
- Reduces the feeling of fullness in the pelvic region
- Non-surgical treatment that is painless and has no downtime
- Provides multiple side benefits such as non-invasive vaginal tightening, enhanced sexual function, and treatment of vaginal dryness


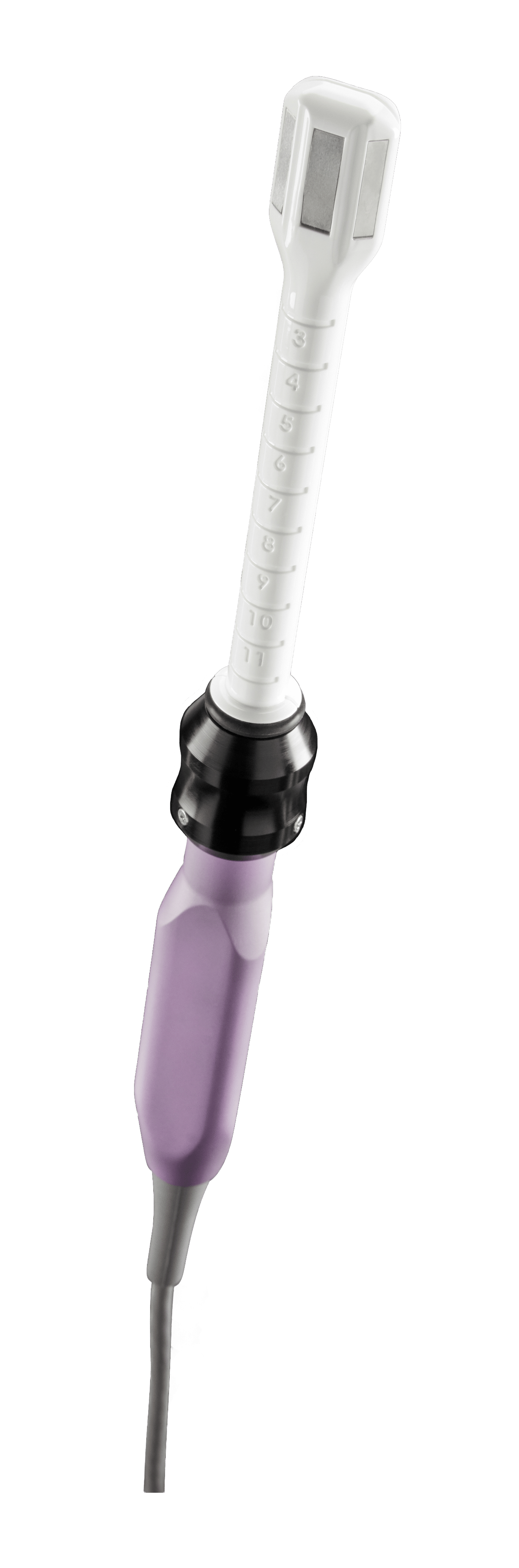
VTone
VTone is an FDA-cleared device that uses intravaginal Electrical Muscle Stimulation (EMS) and neuromuscular re-education to retrain weak pelvic floor muscles in women to treat urinary incontinence.
Benefits of VTone:
- In-office non-invasive procedure to strengthen weak, damaged pelvic floor muscles to improve muscle tone and alleviate urinary incontinence
- The two-sided single use tip is placed easily and comfortably into the vaginal canal
- Restores a patient’s self-esteem and quality of life without bladder mesh surgery or a recovery period
Morpheus8 V
Morpheus8 V utilizes microneedling and radiofrequency energy to strengthen the connective tissue between the vagina and the bladder. By promoting the formation of collagen and elastin molecules, the Morpheus8V handpiece regenerates the thickness of the bladder floor to treat stress urinary incontinence and overactive bladder.
Benefits of Morpheus8 V
- Uses radiofrequency to deliver painless pulses that stimulate collagen and elastin production
- Naturally enhances tissue elasticity, which can improve bladder function and control
- Can also improve symptoms such as vaginal dryness, itching, painful intercourse, and decreased sensitivity
- Minimal recovery period of three to four days with no significant downtime
Emsella
Emsella is a non-invasive procedure that uses electromagnetic energy to painlessly stimulate and strengthen the muscles of the pelvic floor, which can strengthen urinary incontinence.
Patients sit in the Emsella chair during treatment, fully dressed, while the chair emits electromagnetic pulses of energy for 30 minutes. The procedure is entirely painless and can help eliminate the symptoms of urinary incontinence.
O-Shot®
While the O-Shot was originally used to help women improve the quality of orgasms, recent studies have determined that the O-Shot can also be an effective treatment for urinary incontinence. This non-surgical, non-invasive injectable treatment uses your own blood to trigger the body’s natural healing process and stimulate supportive collagen production. The O-Shot is able to improve the symptoms of urinary incontinence, as well as address concerns like vaginal dryness and reduced sensation in the vaginal area.
Benefits of O-Shot:
- Completely natural treatment that uses your own blood to stimulate healing from within
- Can be highly effective for treating stress urinary incontinence
- Can improve other aspects of vaginal function, including a tighter vaginal opening and enhanced sensitivity, as well as a lower orgasm threshold making it easier to achieve climax
What Is the Most Common Cause of Urinary Incontinence in Women?
Damaged and weakened pelvic floor muscles as a result of vaginal delivery, or attempted vaginal delivery prior to cesarean, are the most common causes of female stress urinary incontinence. Poor pelvic floor muscle tone may also have other causes such as being obesity, chronic cough, or surgery that affects the muscles, such as a hysterectomy, or back surgery.
The most common causes of urge incontinence, also known as overactive bladder, are infection, as well as diet choices like caffeine, chocolate, spicy foods, or alcohol.
We Are Here to Help
Dr. Wesley Anne Brady, and the entire staff at Women’s Wellness Institute of Dallas, is an empathetic team who recognizes the emotional toll that urinary incontinence may have on a woman’s self-esteem and social life. They strive to help every patient find the best customized solutions to alleviate physical symptoms and regain their confidence.
Women’s Wellness Institute of Dallas takes a personalized approach to urinary incontinence treatment, offering the best individualized combination of sessions to achieve the greatest advantages from the most up-to-date procedures for your lifestyle demands. Let’s explore your goals and discover the best package for you when you call 214-442-0055 to schedule your consultation.